We offer the widest range of radiation therapy options in the Midwest, allowing our physicians to tailor treatment to each individual patient’s needs.
Our department is one of the largest in the United States and a national leader in developing the most recent radiation treatments for cancer patients. We are the first Department of Radiation Oncology in St. Louis and the Midwest to utilize ultrasound-guided permanent seed prostate implants, high dose rate brachytherapy for a variety of anatomical sites, stereotactic radiosurgery, intensity modulated radiotherapy (IMRT), three dimensional treatment planning, and clinical trials with radioimmunotherapy.
Treatment techniques that have been developed and refined through years of experience are commonly used to treat many of our patients. We constantly review the results of treatment of our patients at the Siteman Cancer Center and periodically refine our treatment policies to maximize cure rates with minimal side effects or toxicity.
Major new equipment projects have seen the introduction of image-guided therapy as part of routine practice and the establishment of a proton treatment facility. These new initiatives provide patients with the latest cutting-edge technology to treat cancer.
Jump to…
- External Beam Radiation Therapy
- 3D Conformal Radiation Therapy (3DCRT)
- Intensity-Modulated Radiation Therapy (IMRT)
- MRI-Guided Radiation Therapy (MR-IGRT)
- Proton Therapy
- Brachytherapy
- Stereotactic Body Radiation Therapy (SBRT)
- Gamma Knife
- Hyperthermia
- Radio-Immunotherapy
- Total Body Irradiation (Bone Marrow Transplantion)
- Total Skin Electron Therapy (TSET)
- Electron Beam Radiation
External Beam Radiation Therapy
The majority of our patients are treated with external beam radiation therapy. This treatment is typically delivered with the use of a linear accelerator, a machine that emits high energy X-rays targeted to the tumor or body region at risk. The duration of treatment ranges from two to eight weeks. The number of treatments will depend on the specific diagnosis and the integration of other treatments such as surgery or chemotherapy.
Before receiving this type of treatment you should know:
- Radiation therapy is not painful; you cannot see or feel the treatment.
- You are required to lie very still for the short duration of treatment.
- The number and pattern of treatments is not an accurate way to judge the severity of your disease. Please ask the physician if you have concerns.
- For your treatments, you will be lying on a table that rises up in the air. The treatment machine rotates around you.
- You are not radioactive after you receive external treatments nor do you pose any health threat to your family and friends
- We encourage you to lead your life as normally as possible. Always ask, if you have questions. Your physician is always prepared to talk over any concerns that you may have about your radiation treatment.
3D Conformal Radiation Therapy (3DCRT)
A modern method of planning and delivering radiation therapy, 3DCRT uses patient specific images to create sophisticated treatments aimed at maximizing radiation dose to the areas that need it while sparing adjacent organs and other sensitive tissues. This technology is allowing Siteman Cancer Center oncologists to increase the cure rate for some cancers and reduce side effects for others. (back to top)
Intensity-Modulated Radiation Therapy (IMRT)
One of the most recent and exciting developments in radiation therapy is intensity modulated radiation therapy (IMRT), which represents a new and increasingly sophisticated method to deliver 3D CRT. Tighter and uniquely shaped radiation dose distributions have the potential to allow greater sparing of critical organs or sensitive tissues. In some cancers of the mouth and throat, IMRT has allowed a high cure rate with sparing of salivary gland function. It is being applied to other cancer sites such as prostate, cervix, soft tissue, lung and brain tumors. Using modern computer dose distribution optimization and dose delivery control, dose distributions can be designed and delivered that more completely spare critical structure, while delivering high doses to the tumors. The equipment uses a computer-controlled multileaf collimator. The radiation treatment is delivered while the accelerator rotates around the patient. The multileaf collimator leaves open and close according to a pattern determined by the computer to deliver the optimal dose distribution. In the case where the leaves are pneumatically actuated, they make a clicking noise as the gantry rotates. Each treatment delivers dose to a 2 centimeter long region, so for treatments of longer tumors, multiple gantry rotations are required. After each rotation, the patient is precisely moved 2 centimeters and the next region is treated. It is very important that the patient remain still during the treatment, as a special immobilization system is used. (back to top)
MRI-Guided Radiation Therapy
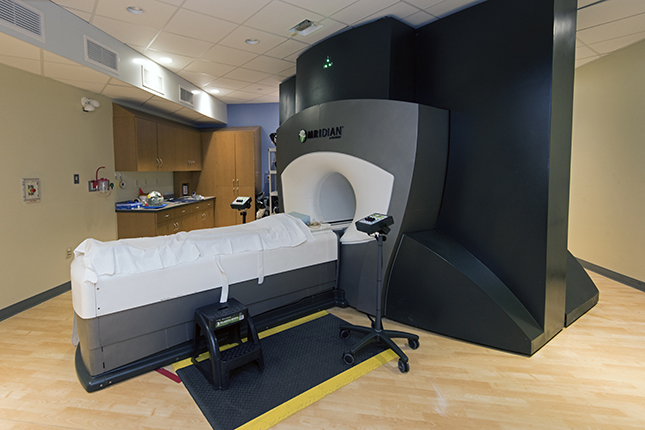
Magnetic resonance image-guided radiation therapy (MR-IGRT) is a treatment method that uses MRI technology to deliver radiation to the treatment site only when it is in exactly the right position. This is especially useful for treating sites in areas of the body that might be affected by things like motion from breathing.
The Department of Radiation Oncology at Washington University School of Medicine began using MRI-GRT with the installation of the ViewRay™ system in 2014, which was developed by a graduate of our medical physics residency program. Our center was the first in the world to use MR-IGRT clinically and to its full capability.
MR-guided therapy allows the physician to have high-quality, large field-of-view images prior to each fraction. This allows fast, online, on-table adaptation of the treatment plan. Our system is also capable of real-time imaging and tracking of tumors during treatment to ensure accurate delivery.
Unlike imaging techniques such as CT scans or X-rays, magnetic resonance imaging (MRI) does not use radiation. Instead, the MRI machine creates a strong magnetic field that is used along with radio waves to create an image of the soft tissues inside of your body.
MR-IGRT also allows your treatment team to use a technique called online adaptive radiotherapy. This means that your treatment plan can be re-evaluated and, if necessary, revised by your physician you are at the machine, minutes before your actual treatment.
Proton Therapy
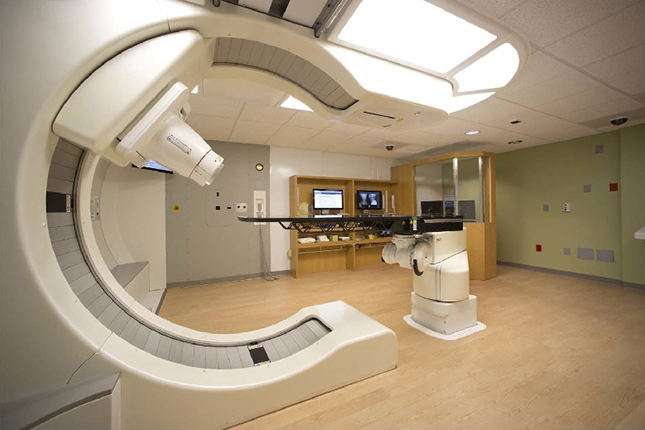
The S. Lee Kling Center for Proton Therapy at Siteman Cancer Center opened in December 2013, and is the world’s first single-room proton therapy facility, and the first and only proton therapy center located in Missouri. Due to its location adjacent to the Center for Advanced Medicine, patients undergoing proton therapy treatment have easy access to multidisciplinary care.
Our facility uses the world’s first compact proton accelerator, the Mevion S250™, and our staff has been instrumental in developing treatment planning and quality assurance processes for users of this machine all over the world.
March 16, 2020 – Siteman Cancer Center announces new Proton Therapy Director
Like standard radiation therapy, proton therapy is painless. Protons enter the body and destroy cancer cells and tumors. What makes proton therapy unique is the ability to control the depth and shape of the beam of radiation, allowing your proton treatment team to deliver less radiation to normal tissues than other forms of external radiation. Areas past the beam’s stopping point will receive little to no radiation. This level of control is especially advantageous when treating tumors near the heart, brain, and spine, and can often allow physicians to treat tumors that standard radiotherapy methods cannot.
Proton for pediatric patients
Proton therapy can be especially beneficial when treating pediatric cases due to its ability to spare patients from receiving excessive radiation to normal tissues. For patients requiring craniospinal radiation, proton therapy can spare anterior organs such as heart, lung, liver, bowel, esophagus, thyroid, and bladder. For patients requiring boosts, proton therapy is capable of preserving hearing and cognitive function for pediatric patients by avoiding important parts of the inner ear and brain.
Proton for lung patients
Radiation is an important ingredient in the recipe for fighting lung cancer. It has been demonstrated in a variety of clinical trials that physicians can use proton therapy to deliver highly conformal dose to the tumor without excessive toxicity to the surrounding normal tissue, including healthy portions of the lung, heart, and esophagus. The ability to reduce radiation exposure to the healthy parts of the lungs allows physicians to escalate radiation dose to tumors without increasing the toxicity.
Proton for brain (intracranial and base-of-skull patients)
Proton therapy is widely accepted as a very effective treatment in eradicating brain tumors while preserving the normal function of the brain. Brain tumors are typically surrounded by structures such as the brain stem and optic nerves, that are critical for maintaining vital functions. By carefully selecting angles and precisely controlling the range of protons, oncologists are able to preserve the functions of these important areas.
Proton for head and neck patients
The precise nature of proton therapy makes it an excellent option for the treatment of head and neck cancers. Since proton therapy offers physicians extremely precise control over the beam, critical structures such as the spinal cord, salivary glands, and jawbone can receive much lower doses of radiation while a patient’s tumor is treated, which can help some patients avoid side effects such as permanent dry mouth or bone injury.
Proton for prostate patients
Radiation therapy outcomes for prostate cancer rival the best surgical series. In a randomized trial conducted in the United Kingdom, patients that were treated with radiation therapy had equivalent cancer free survival rates as patients that had radical prostate surgery. Proton therapy is one of many ways to deliver highly precise radiation therapy for prostate cancers that are localized to the prostate gland. Doctors at the Siteman Cancer Center are collaborating with other proton centers to study whether proton therapy could offer any clinical advantage over modern x-ray therapy.
Brachytherapy
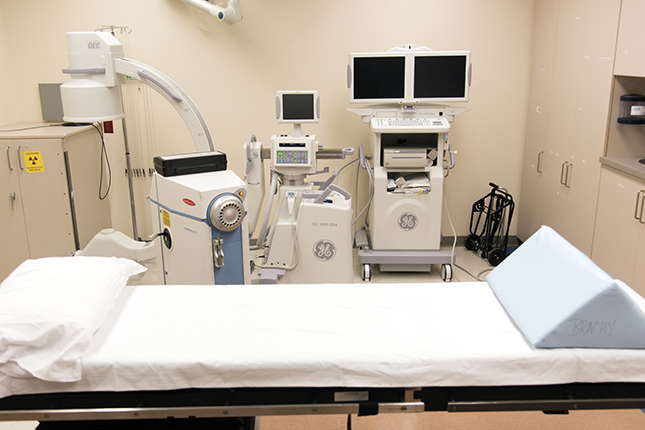
Our brachytherapy program is one of the largest and most comprehensive in the United States, delivering more than 1000 treatments annually. Brachytherapy refers to the placement of radioactive sources directly into the body to treat cancers. Often the procedure involves placement of devices, tubes or catheters to hold the radioactive sources temporarily for a few hours or days. In other circumstances, the sources are placed into a tumor and left there permanently.
Brachytherapy allows the radiation oncologist to deliver very high radiation doses to small volumes of cancer without treating adjacent organs or sensitive tissues. In addition to treating cancer with X-ray photons and electrons directed to the tumor area from outside the patient, the Department of Radiation Oncology also uses procedures that allow the therapeutic radiation to be directed from inside the patient, often close to or within the tumor using sealed sources of radioactive material inserted in hollow tubes or catheters placed in the desired area.
Our brachytherapy program also includes “radiopharmaceutical therapy” using liquid radioactive chemical compounds which the patient drinks or receives through injection. These radioactive liquids are localized in the tumor area.
Brachytherapy procedures carried out in the Department of Radiation Oncology include treatment of cancer of the vagina, cervix and uterus with radioactive iridium, treatment of cancers in the breast, esophagus and soft tissues with radioactive iridium, and treatment of cancer of the prostate with radioactive iridium, iodine and palladium, and treatment of cancer in the eye with radioactive iodine. Our radiopharmaceutical therapy procedures include treating cancer of the thyroid with an orally administered salt solution of radioactive iodine, metastatic tumors of the bone with an intravenously injected solution of radioactive radium or samarium, and treatment of tumors in the liver with radioactive yttrium microspheres.
Brachytherapy for gynecologic cancer
Many cancers of the cervix and uterus are treated with combinations of external beam radiation therapy and brachytherapy. Special devices are placed in the uterus or vagina, or adjacent to the location of the cancer. Radioactive sources are then placed inside these devices to deliver a highly focused and controlled dose of radiation to the cancer. In high-dose rate (HDR) radiation treatments, the radioactive sources are placed for just several minutes. These treatments may be repeated 3 to 6 times over the course of a few weeks.
Brachytherapy for breast cancer
Many cancers of the breast are treated with a combination of surgery paired with either external beam radiation therapy or brachytherapy. For patients receiving brachytherapy, after removal of the tumor in surgery, special treatment devices are placed in the tumor bed, or adjacent to the location of the tumor bed. Radioactive sources are then placed inside these devices to deliver a highly focused and controlled dose of radiation to the tumor bed. In high-dose rate (HDR) radiation treatments, the radioactive sources are placed for just several minutes. These treatments may be repeated 10 times, twice daily, over the course of 5-7 days.
Brachytherapy for prostate cancer
An increasingly popular alternative to radical prostatectomy is prostate brachytherapy. Using ultrasound and X-ray guidance, radioactive sources, smaller than a grain of rice, are inserted directly into the prostate gland during anesthesia. These radioactive Iodine or Palladium seeds remain in the gland permanently and give very high radiation doses to the prostate with acceptably low rates of side effects. Cure rates are comparable to radical prostatectomy and external beam radiation therapy for appropriately selected patients. Recently, high dose rate (HDR) brachytherapy has been introduced as an alternative to permanent seed implant. Your radiation oncologist can help decide which treatment is best for you.
Brachytherapy for ocular melanoma
This rare form of cancer can be treated effectively with brachytherapy or protons. With the ophthalmologist, a special device or plaque is placed against the eye where these tumors grow. This device is left in place for several days and delivers a high radiation dose to a very small area. This treatment allows the ophthalmologist to cure the melanoma without radical removal of the eye.
Other uses of brachytherapy
Brachytherapy is used in several other types of cancers on an individual basis. Radiation oncologists at the Siteman Cancer Center have successfully used both high dose rate (HDR) and low dose rate (LDR) brachytherapy to treat patients with malignant tumors of the head and neck and soft tissues (sarcomas).
Stereotactic Body Radiation Therapy (SBRT)
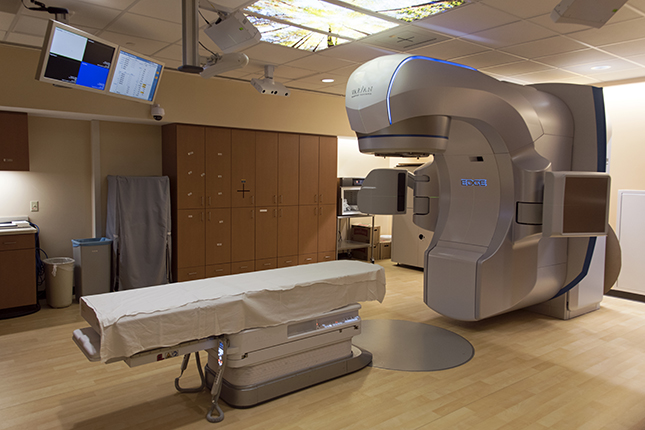
Stereotactic Body Radiation Therapy (SBRT) specifically refers to a procedure whereby radiation is precisely aimed at a focal point or tumor. The dose distributions achieved by these techniques assure large doses to the target volume and much lower doses to the surrounding normal tissues. Stereotactic body radiation is 5 or fewer treatments.
SBRT is often used for brain, lung, liver, heart, and prostate cancers.
Once the images are obtained, they are transferred to a computer that is used for treatment planning. This may take one to several hours depending on the complexity of the treatment plan. During the treatment planning process, the sizes and directions of all radiation beams, and the dose to be given are determined by the radiation oncologist, physicist and dosimetrist, and in certain cases, the referring provider (surgeon, pulmonologist, etc.). Dose to the treatment volume and healthy tissues are calculated and displayed graphically on the computer screen. The computer simulates the treatment before it is actually given. A number of potential plans are compared. The best plan is chosen that maximizes the dose in the disease site but minimizes the dose to healthy tissues. In this way, we create a specific treatment plan, tailor-made for each patient. The computer then prints out a record that describes how the plan is to be performed on the radiation treatment machine.
Following computerized planning, the radiation treatment machine is made ready for the patient. The patient arrives in the treatment room, lies on a special motorized table and is lifted toward the treatment position. The patient is carefully moved into a position that puts the disease site where the radiation beams will be directed. The patient’s position is double-checked by the physician and physicist, during which time the patient will hear the coordinates, or numbers, as they are being read from the treatment machine.
Once the patient position is verified, all but the patient leave the room before the radiation beam is turned on. When the radiation beam is on, the patient will hear a humming sound coming from the machine. This is normal and provides an audible indication that the radiation beam is activated. The beam may be turned off and on repeatedly and the patient may be repositioned several times depending on the complexity of the treatment plan. During the entire treatment process, the patient is watched by the therapist using two video cameras in the treatment room. An intercom system also is used. The patient can signal to the therapist operating the treatment machine at any time to halt the treatment if needed.
Gamma Knife
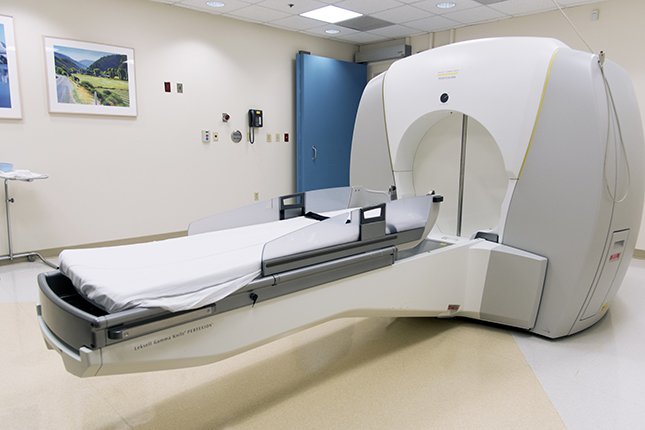
Gamma Knife stereotactic radiosurgery is a well-established treatment method used to treat several conditions or diseases affecting the brain. In clinical use since 1968, over 500,000 patients have been treated worldwide, and over 60,000 patients worldwide receive this treatment each year.
The Gamma Knife isn’t actually a knife at all. It is a machine that uses gamma rays produced by nearly 200 cobalt-60 radiation sources to target and destroy abnormalities within the brain with extremely high accuracy and precision. The result is like a pinpoint of radiation so small and powerful it can reach the specific part of the brain that needs treatment without destroying healthy surrounding tissue. The doctor makes no incisions in your head and the treatment itself is painless. A team made up of a neurosurgeon, radiation oncologist and medical physicist direct these treatments.
The individual beams are too weak to damage healthy tissue on their way to the target area, but become very powerful as they simultaneously merge at a single focal point. By placing a patient’s head in one or several positions, the shape and dose of radiations is optimized to affect only the target, avoiding any damage to the surrounding healthy tissue. In most cases, patients receive a single treatment.
Gamma knife treatments allow the stereotactic therapy to be done in less time. In addition, the gamma knife can treat very small lesions (4-5 millimeters) and functional neurologic disorders such as epilepsy, trigeminal neuralgia, essential tremor, and others.
The treatment process
The treatment consists of four main steps – attaching the frame, imaging, treatment planning and treatment. During the procedure, different members of the team (consisting of a neurosurgeon, radiation oncologist, medical physicist, neuroscience nurse, and radiation therapist) will monitor your care and you most likely will remain awake at all times. If you have a favorite music, you may listen to it during treatment.
Attaching the frame
To begin the procedure, your neurosurgeon will spend a few minutes placing your head in a lightweight frame. Your hair does not need to be cut or shaved. A local anesthetic will be applied where the frame is to be attached. You will experience some discomfort for a short period of time from the injections of anesthetic. Once the anesthetic has taken effect, the frame is secured with four pins that go tightly against your skull, in order to stabilize your position during imaging and treatment. With the frame placement there is some discomfort, but local pain medicine makes this minimal. Patients usually say the frame looks far worse than the actual experience. Once the frame adapter is attached, the patient will lie down on the treatment couch.
Your head will remain in the frame throughout the entire procedure. The frame adapter immobilizes the patient’s head and moves it from position to position. This automatic positioning helps expedite the procedure and allows treatment of the lesion with pinpoint accuracy.
Imaging
Once your head frame is in place and measurements are taken, it’s time for imaging. A coordinate box is used during imaging to provide reference points on the images for the treatment plan. Although you may have previously done these imaging studies, they need to be completed with the frame on to precisely define the location, size and shape of the area to be treated. Once the images are done they are transferred to a sophisticated treatment-planning computer.
Treatment planning
While you rest, read, or watch TV, your neurosurgeon, radiation oncologist, and medical physicist will prepare a three-dimensional treatment plan customized for your condition utilizing specially designed software. Once this plan is re-checked and approved, treatment can begin.
Treatment
Your doctor will then tell you how long the actual procedure will take. The treatment itself is totally silent and painless. The frame adapter is attached and the patient will lie down on the treatment couch. During the course of your treatment, you will remain fully awake and can communicate with your radiation therapist and nurse through an audio/video connection. Remember, members of your treatment team are close at hand to assist if needed.
Once you’ve finished treatment, the frame will be removed. Occasionally, some patients experience a slight headache or mild swelling where the frame was attached. For most patients, there is no such effect.
You will be given discharge instructions and depending on your specific diagnosis and areas treated, your doctor will discuss with you and your family any precautions or possible side-effects that may occur as well as treatment options for them.
Your doctor will schedule follow-up visits and consultations, some with repeat MRI or CT scans, to monitor your progress. Because the effects of treatment occur over time, it may take weeks or even months to see the full results of your treatment. As always, consult your doctor should you have any questions or concerns regarding your condition.
For more information on this type of treatment, please visit Gamma Knife of St. Louis.
Hyperthermia Therapy


Local heating of tissue has been known to be an effective treatment against a number of cancers, especially in combination with radiation and chemotherapy. Radiation is delivered as soon as possible either before or after the heat to increase the effectiveness of the radiation without increasing the dose of radiation administered to the patient. Chemotherapy can also be infused before or during the heating.
Washington University School of Medicine, Department of Radiation Oncology has been using heat to treat tumors since 1981, when the Hyperthermia Treatment Center opened as the first in the Midwest and one of the most advanced centers of this kind in the country.
Hyperthermia heats tumors to mildly elevated temperatures. This heating will cause some of the cancer cells to die, but more importantly, it makes the cells that have survived more susceptible to the curative effects of radiation therapy. The heat treatments can be administered with either ultrasound, radiofrequency, or even microwaves. Often, the radiation oncologist will need to place a temperature monitor inside the treatment site to measure the temperature and to make sure the site is heated to the target temperature for an appropriate duration. Once the target temperature is reached, the tissues are maintained at that temperature for approximately 15 minutes.
Most centers do not offer hyperthermia, and the fact that we still provide this important treatment sets the Department of Radiation Oncology at Washington University apart from other cancer treatment centers in the Midwest. We have one of the longest standing hyperthermia programs in the nation, and have recently invested in new technologies to heat deeper tumors that will be the subject of future research.
Currently, we use hyperthermia to treat breast cancers that have recurred on the chest wall following prior surgery. Occasionally we will use it to treat other superficial cancers that have not responded to other more common treatment approaches like surgery, radiation, or chemotherapy.
Radio-Immunotherapy
Antibodies directed at cancer cells have been linked to radioactive atoms. These antibodies seek and attach themselves to the cancer cells and deliver a toxic radiation dose to the tumor. These treatments are available for some lymphomas. Radiation oncologists and medical oncologists work together in delivering this therapy. (back to top)
Total Body Irradiation (Bone Marrow Transplantion)
Bone marrow transplantation is used to treat many types of cancer, including leukemia and lymphomas. Total body irradiation (TBI) is frequently used to prepare patients to accept donated marrow. TBI eliminates the patient’s own marrow along with the malignant cells. It also suppresses their immune system to allow safe engraftment of the new healthy bone marrow. A bone marrow transplant specialist will work with our radiation oncology staff to decide when TBI is appropriate for a patient and coordinate the proper timing and radiation dose. (back to top)
Total Skin Electron Therapy (TSET)
Total skin electron therapy (TSET) is a treatment method that uses electron beams to deliver radiation to the entire body surface, but only superficially. This is especially useful for treating lymphomas that involve the skin, like mycosis fungoides. The goal is to treat the entire skin volume with a uniform amount of radiation dose while minimizing side effects. Washington University has used TSET for several years. This technically challenging treatment method is not offered at very many institutions and we are proud to be able to offer it for our patients. We aim to achieve complete disease remission while providing maximum comfort for our patients during the procedure. (back to top)
Electron Beam Radiation
Electron beam radiation is type of radiation that is well suited to treating superficial cancers because electrons do not penetrate very deep into body tissues. With electrons, a superficial tumor can be treated while protecting the healthy cells deeper in the body. It is often used at Washington University to offer a non-surgical management option for skin cancers like basal cell carcinomas and squamous cell carcinomas.
Electron beam radiation is especially useful to treat cancers located near the eyes, ears, nose, or lips, because it can produce favorable cosmetic outcomes. It is often recommended as a treatment option when surgery might otherwise leave a less desirable cosmetic outcome or when patients cannot undergo surgery for their skin cancer because of other medical conditions.