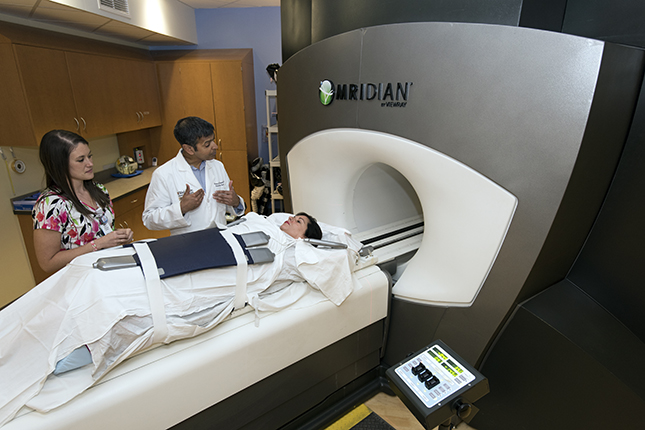
Parag Parikh, MD, an associate professor of radiation oncology at Washington University, will be the lead investigator on a multi-center clinical trial studying pancreatic cancer patients who receive treatment on an MR-guided linear accelerator system called the ViewRay MRIdian® Linac. The study will be available in multiple centers in the U.S., Europe and Asia.
The trial was initiated after promising trends were found in a retrospective review of 42 patients from Washington University; University of California, Los Angeles; University of Wisconsin, and VU University Medical Center Amsterdam. The data reviewed showed that the patients with unresectable pancreatic cancer that received a higher, but more targeted, dose of radiation therapy to their disease site had lower toxicity rates and better rates of survival.
This new trial will follow pancreatic cancer patients whose tumors have grown too large to be surgically removed, but have not spread to other parts of the body. The patients will undergo online, adaptive MRI-guided radiotherapy (MRgRT). The therapy uses MRI moments before the treatment to determine the positions of the tumor and surrounding structures, allowing the physician to adapt the treatment each day to match the precise location of the organs. MRI treatment control, a process that uses MRI technology to monitor tumor movement during the treatment, allowing the team to deliver the treatment beam only when the tumor is exactly in place, improves accuracy of tumor targeting.
“I think the use of online, adaptive MR guided radiation therapy for pancreatic cancer has great potential to deliver ablative doses of radiation to the pancreas,” says Dr. Parikh. “It’s the first time we are giving the pancreas the same radiation dose that we give to lung and liver tumors, and it has the chance to improve the outcomes of these patients.”
The radiation oncology program at Siteman Cancer Center at Barnes-Jewish Hospital and Washington University School of Medicine was the first in the world to clinically implement MRgRT technology, and continues to be the only institution in Missouri and the surrounding area to offer this form of radiotherapy. As a result, therapists, dosimetrists, nurses, physicists and physicians in the department have exceptional experience with the use of this technology. A pioneer in the development of MR-guided adaptive treatment, and especially its use for pancreatic cancer, the Department of Radiation Oncology will have two treatment machines with the ability to deliver MRgRT by 2018.
Siteman Cancer Center also operates one of the largest and most experienced programs in the nation for use of MRI imaging in the planning stages for radiation therapy. In a process called MRI-Simulation, physicians use magnetic resonance imaging to better visualize some tumors in order to improve delivery of radiation to only the tumor site and not to the surrounding organs.
Read more
MR linac radiotherapy allows for successful high-dose pancreatic cancer treatment (DOTmed) »